May is Skin Cancer Awareness month and we are glad to partner with you in educating patients. Below is a brief summary of the most common skin cancers that you may want to forward to your patients.
As a diagnostic laboratory with a major focus on skin cancer, we are proud to serve providers across the United States in the care of their patients with skin disease. The most common skin cancers are basal cell carcinoma, squamous cell carcinoma and malignant melanoma. Each of these has different clinical presentations, treatment options and prognoses.
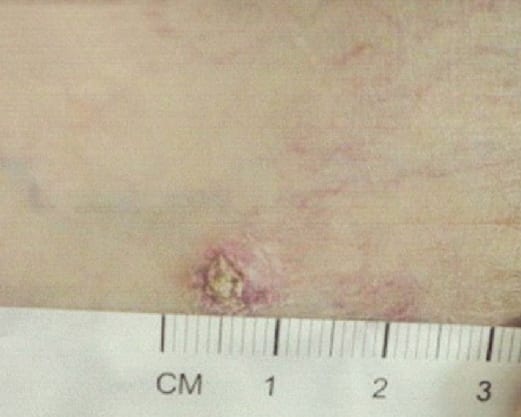
Basal Cell Carcinoma
Basal cell carcinoma is the most common skin cancer. It can occur anywhere on the body, but the most common location is the face, particularly the nose. The lesion is associated with chronic sun exposure, and it is most common in patients with fair skin who have had long term exposure to ultraviolet radiation. These are slow growing lesions that often have a shiny “pearly” appearance or may present as a bump or skin ulcer that does not heal. Basal cell carcinoma typically does not spread (metastasize), but if left untreated, the tumor can destroy normal tissue and structures, such as the nose, eyelid, or ear. Early surgical excision is the best treatment, although there are destructive modalities as well.
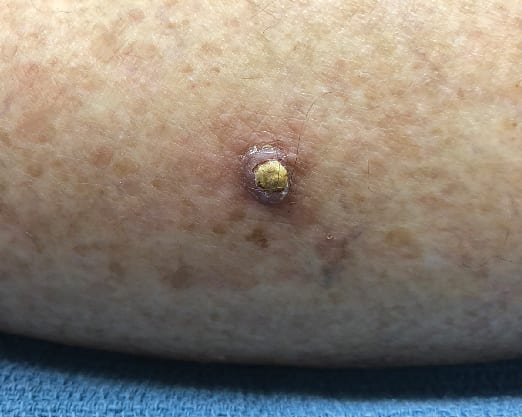
Squamous Cell Carcinoma
Squamous cell carcinoma is the next most common skin cancer variant. It also occurs on sun exposed skin with a predilection for the head and neck areas, but it can also occur on the extremities or trunk. A subset of squamous cell carcinoma, known as keratoacanthoma, may develop quickly. The lower leg is the most common location for keratoacanthoma. Squamous cell carcinoma is also associated with chronic ultraviolet radiation and is more common in fair skinned individuals (but anyone can be at risk). These are locally destructive, but also may metastasize on occasion, if left untreated. Patients with a compromised immune system may have more aggressive tumors.
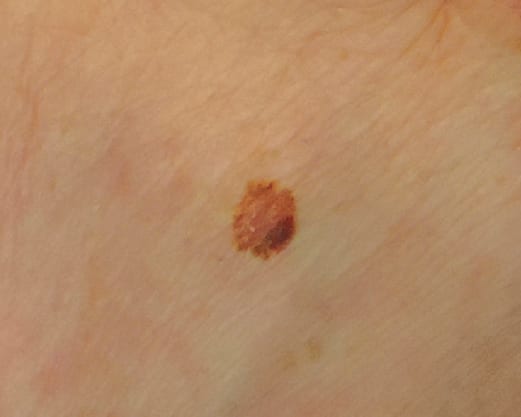
Malignant Melanoma
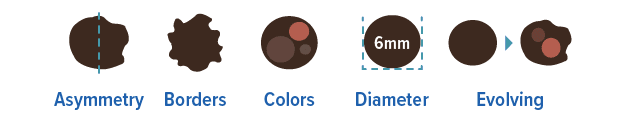
Malignant melanoma is less common (accounting for 1 percent of skin cancers), but it is one of the fastest growing skin cancers in terms of prevalence. It is estimated that 1 in 38 Caucasian people in the U.S. will develop melanoma in his or her lifetime (with a lower prevalence in people of color). Melanoma risk increases with age, but new diagnosis of melanoma is not uncommon in young adults. Risk is highest in people with fair skin, light eyes, multiple nevi (moles), and history of multiple sunburns as a child. Family history of melanoma in a first degree relative is also a risk factor. The clinical presentation is usually a mole that has changed or grown and is irregular in appearance. The ABCDE’s (Asymmetry, Irregular Borders, Color variation, Diameter 6 mm or greater, and Evolution of the lesion) are used to diagnose the lesion. Early diagnosis and treatment are key to curing the disease, as melanoma may be fatal, even in its earlier stages.
The most important preventative measures are daily sunscreen use, wearing UV protective clothing and hats, avoidance of sun exposure, particularly during peak hours, and avoidance of tanning booths. Skin self-examination is helpful to prevent the disease and diagnose lesions early. If you are concerned about suspicious or changing lesions, we recommend to see a dermatologist.

